Ankle Pain Treatment in Tel Aviv
- Healing timeline: Grade I sprain 1-3 weeks, Grade II 3-6 weeks, Grade III 6-12 weeks; return to sport typically 6-8 weeks with active rehab
- Functional vs immobilisation: functional treatment returns patients to sport 7 days faster than immobilisation (Kerkhoffs et al., Cochrane 2012)
- Avoiding chronic instability: ~40% develop chronic ankle instability after a sprain; neuromuscular peroneal training cuts recurrence by 52% (Gribble et al., 2016)
- X-ray needed? Ottawa Ankle Rules have 100% sensitivity for fracture and reduce unnecessary X-rays by 36% (Stiell et al., JAMA 1994) — most sprains start physio immediately
- Cost: ₪400 flat per 50-60 min 1:1 session with Alejandro Zubrisky BPT (MoH license 10-120163), no deposit
- Where & when: Yaakov Apter 9, Tel Aviv · Sun-Thu 07:00-22:00, Fri 07:00-14:00 · ★5.0 across 190+ verified reviews
Comprehensive physiotherapy for ankle sprains, chronic ankle instability, Achilles tendinitis, and plantar fasciitis. Functional rehabilitation using the Ottawa Ankle Rules, proprioceptive training, and eccentric loading protocols.
Is my ankle pain a sprain or something else?
Not all ankle pain is a sprain. About 85% of ankle sprains are lateral sprains of the ATFL, CFL and PTFL complex, but medial deltoid injuries, Achilles tendinopathy, and plantar fasciitis are also common. Plantar fasciitis alone affects 10% of people over a lifetime. Accurate differential diagnosis guides effective treatment.
The ankle is a complex weight-bearing joint subject to high forces during walking, running, and jumping. Ankle sprains account for 15-20% of all injuries in the general population and up to 45% in athletic populations. Approximately 85% of ankle injuries are lateral ankle sprains involving the anterior talofibular ligament (ATFL), calcaneofibular ligament (CFL), and posterior talofibular ligament (PTFL) complex.
However, ankle pain isn't always a sprain. Medial ankle injuries (deltoid ligament), Achilles tendinopathy, and plantar fasciitis are common causes. Plantar fasciitis alone affects 10% of the population over a lifetime. The key to effective treatment is accurate differential diagnosis and targeted intervention.
Common Ankle Pain Causes
- Lateral Ankle Sprain: 85% of ankle sprains; ATFL/CFL/PTFL injury; Grade I-III classification
- Chronic Ankle Instability: 40% develop after initial sprain; neuromuscular control deficiency
- Medial Ankle Sprain: Deltoid ligament; less common; high-energy mechanism; often with fibular fracture (Maisonneuve)
- Achilles Tendinopathy: Affects 6-18% of runners; midportion or insertional; eccentric loading responsive
- Plantar Fasciitis: Most common heel pain (10% lifetime prevalence); heel fat pad atrophy; morning stiffness
Ankle Anatomy and Regional Structures
ATFL + CFL + PTFL Ligament Complex
Incidence: 85% of ankle sprains
- Anterior Drawer Test — 90% sensitivity Grade III
- Talar Tilt Test — assesses ankle inversion stability
- Ottawa Rule: tenderness at posterior fibula or lateral malleolus tip
- Most common injury mechanism: inversion + plantarflexion
Deltoid Ligament (Superficial + Deep)
Incidence: Less common; high-energy
- Often with proximal fibula fracture (Maisonneuve)
- More inherently stable than lateral
- Eversion injury mechanism
- Higher force required for injury
Achilles Tendon + FHL + Posterior Impingement
Prevalence: 6-18% of runners
- Midportion (non-insertional) most common
- Os trigonum syndrome in dancers/kickers
- FHL tenosynovitis with tight ankle
- Eccentric loading 90% success rate
Plantar Fasciitis + Heel Fat Pad
Prevalence: 10% lifetime; most common heel pain
- Plantar fascia-specific stretch 65% success
- Heel fat pad atrophy from aging/loading
- Calcaneal stress fracture consideration
- Baxter's nerve entrapment can coexist
Do I need an X-ray after an ankle injury?
You need an X-ray only if the Ottawa Ankle Rules are positive: malleolar-zone pain plus tenderness at the posterior fibula tip, posterior tibia tip, or inability to bear weight for four steps. These rules have 100% sensitivity for fractures and cut unnecessary X-rays by 36%, avoiding needless radiation.
The Ottawa Ankle Rules have 100% sensitivity for detecting fractures and reduce unnecessary X-rays by 36%. Use them immediately after ankle injury to determine if imaging is needed. The rule states: X-ray the ankle if there is pain in the malleolar zone AND any of these criteria: (1) tenderness at posterior fibula tip, (2) tenderness at posterior tibia tip, (3) inability to bear weight immediately and for four steps.
These rules prevent unnecessary radiation exposure while ensuring fractures aren't missed. Our physiotherapists are trained in Ottawa Rule assessment and will refer for imaging when indicated.
How is an ankle sprain rehabilitated step by step?
Modern care uses POLICE (Protection, Optimal Loading, Ice, Compression, Elevation) instead of full rest. Rehab progresses in four phases: protection and pain-free loading on days 1-3, controlled movement on days 3-7, strengthening and proprioception at weeks 2-4, then sport-specific agility and return-to-sport work at weeks 4-8.
Modern ankle sprain management has evolved from RICE (Rest, Ice, Compression, Elevation) to POLICE (Protection, Optimal Loading, Ice, Compression, Elevation). This emphasizes controlled movement and graduated loading rather than immobilization.
Phase 1: Days 1-3 (POLICE)
- Protection: ankle support/wrap, crutches if needed for full weight-bearing pain
- Optimal Loading: pain-free weight-bearing as tolerated
- Ice: 15-20 minutes every 2-3 hours for inflammation
- Compression: elastic wrap to reduce swelling
- Elevation: above heart level for 48 hours
Phase 2: Days 3-7 (Controlled Movement)
- Gentle ankle ROM: plantarflexion, dorsiflexion, inversion (pain-free only)
- Isometric strengthening: intrinsic ankle muscles without movement
- Weight-bearing progression: 25%, 50%, 75%, 100% load
- Proprioceptive training: single-leg stance on firm surface
Phase 3: Weeks 2-4 (Strengthening)
- Resistance strengthening: peroneal muscles (eversion), tibialis anterior, calf
- Proprioceptive training progression: foam surface, BAPS board, wobble board
- Balance training: single-leg stance on unstable surface; eyes closed
- Gait retraining: normalize walking pattern
Phase 4: Weeks 4-8 (Sport-Specific)
- Running progression: walk-run intervals, progress to continuous running
- Agility training: figure-8 running, cone drills, cutting movements
- Plyometrics: single-leg hops, bounding, lateral bounds (if sports-relevant)
- Return-to-sport assessment: functional movement screening
How can I stop my ankle from spraining again?
About 40% of people who sprain their ankle develop chronic instability with recurrent sprains. A landmark 2016 RCT found neuromuscular training reduces recurrence by 52% at six months. Prevention combines peroneal eversion strengthening, proprioceptive BAPS and wobble board progression, balance work, and sport-specific reactive drills.
Forty percent of individuals who sustain a lateral ankle sprain develop chronic ankle instability (CAI) — characterized by recurrent sprains and instability sensation. A landmark 2016 RCT found neuromuscular training reduces recurrence by 52% at 6 months compared to no training.
CAI Prevention Program
- Peroneal Muscle Retraining: Eversion strengthening with resistance; lateral stability focus
- Proprioceptive Training: BAPS board progression (firm → soft → unstable); wobble board; single-leg stance eyes closed
- Balance Training: Tandem stance, single-leg stance with arm reach, perturbations
- Functional Stability: Sport-specific movements; reactive drills
How is Achilles tendinopathy treated?
Achilles tendinopathy affects 6-18% of runners and responds well to the Alfredson eccentric loading protocol, which achieves 90% clinical success. You lower the affected leg over a step edge in dorsiflexion across three seconds, performing 15 reps by 3 sets twice daily for a minimum of 12 continuous weeks.
Achilles tendinopathy affects 6-18% of runners. The Alfredson eccentric loading protocol achieves 90% clinical success. This involves plantarflexing the calf over a step edge (load the tendon in lengthened position) and lowering with control over 3 seconds. Performed twice daily for 12 weeks, this mechanical loading stimulus promotes tendon remodeling and healing.
Eccentric Loading Protocol (Alfredson)
- Position: stand on step edge, plantarflex (rise up on toes using both legs)
- Movement: remove healthy leg, lower affected leg over 3 seconds in dorsiflexion
- Repetitions: 15 reps × 3 sets, twice daily (morning and evening)
- Progression: add load (hold dumbbell) when pain-free
- Duration: minimum 12 weeks continuous protocol
Plantar Fasciitis Treatment
Plantar fasciitis causes 10% lifetime prevalence of heel pain. A 2003 RCT (n=101) compared two stretching protocols: plantar fascia-specific stretch versus Achilles stretch. Plantar fascia stretch achieved 65% excellent results at 8 weeks versus 53% for Achilles stretch alone.
Plantar Fascia-Specific Stretch
- Position: seated, knee extended, grasp toes
- Movement: pull toes toward shin (dorsiflex foot, creating arch tension)
- Duration: hold 30 seconds × 3 reps, 3 times daily
- Timing: especially before first steps in morning
- Progression: plantarflex ankle against resistance for strengthening
Red Flag for Stress Fracture: If ankle pain is localized to the calcaneus (heel bone), worsens with impact, and is unresponsive to conservative care after 6 weeks, suspect calcaneal stress fracture. This requires imaging and may need immobilization. Don't ignore persistent heel pain.
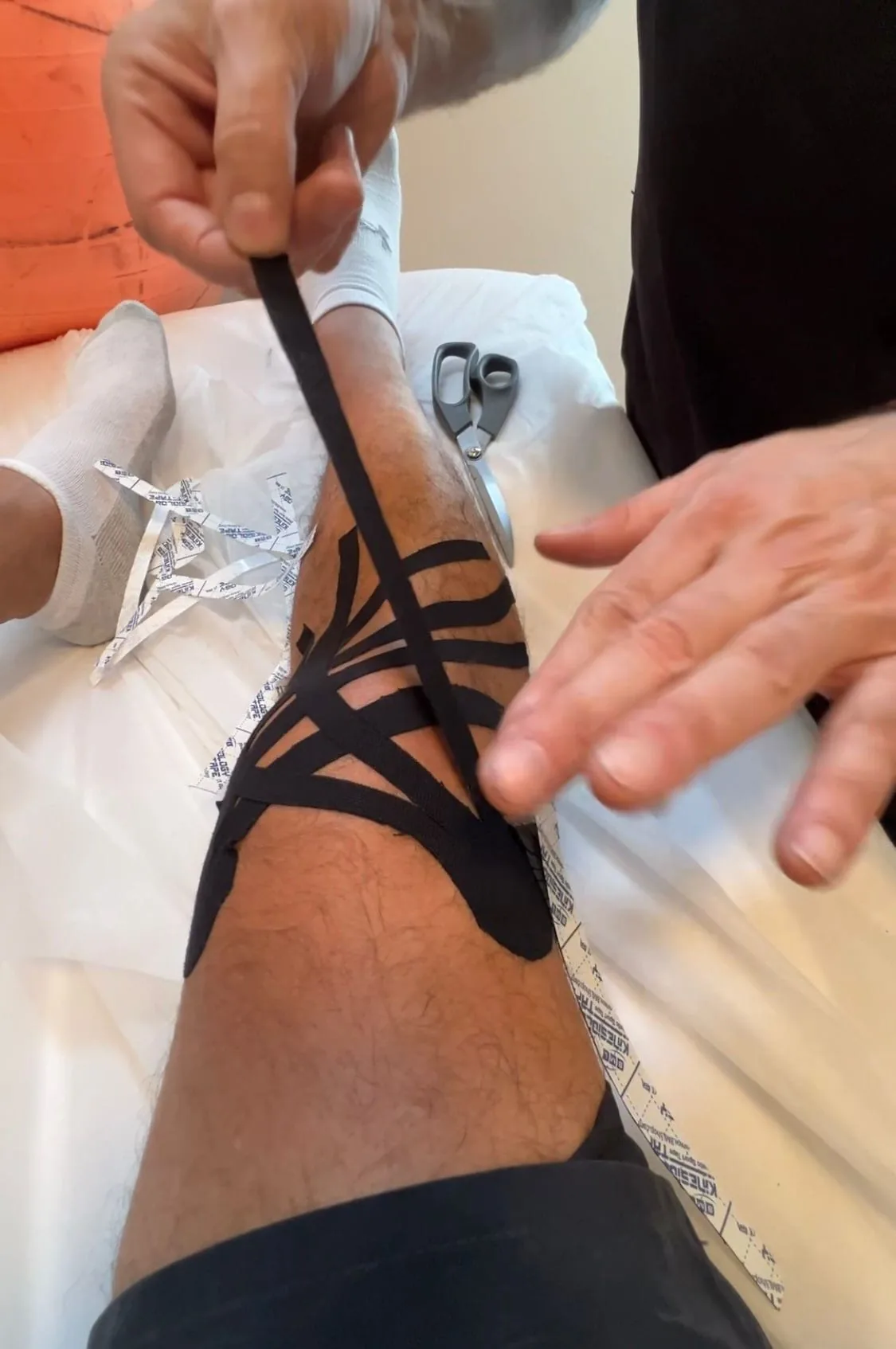
Ankle Taping vs Bracing for Return to Sport
Both taping and bracing improve ankle proprioception and reduce re-injury risk. Research shows both are effective, with individual preference dictating choice. Bracing allows earlier return to activity in Grade II-III sprains due to superior support. Taping requires frequent reapplication during athletic activity.
How long until I can return to sport?
Return-to-sport time depends on the injury. Grade I sprains take 2-4 weeks, Grade II take 4-6 weeks with structured rehabilitation, and Grade III take 8-12 weeks with possible surgical referral. Achilles tendinopathy needs 8-12 weeks with eccentric loading, and plantar fasciitis 4-8 weeks with stretching and strengthening.
- Grade I (Mild Sprain): 2-4 weeks to return to sport
- Grade II (Moderate Sprain): 4-6 weeks with structured rehabilitation
- Grade III (Severe Sprain): 8-12 weeks; potential surgical referral
- Achilles Tendinopathy: 8-12 weeks with eccentric loading protocol
- Plantar Fasciitis: 4-8 weeks with stretch + strengthening
Rapid Return to Sport and Activity
Our evidence-based ankle rehabilitation gets athletes back safely and faster. Functional progression, proprioceptive training, and sport-specific preparation restore full capacity. Start your ankle recovery today.
Research Evidence Supporting Ankle Treatment
- Kerkhoffs et al. (Cochrane 2012, CD000380): Functional treatment vs immobilization for ankle sprain: faster return to activity (7 days sooner), better ROM at 3 months, no difference in re-injury rate
- Gribble et al. (J Athletic Training 2016, PMID 27501368): 40% of lateral ankle sprains develop chronic instability; neuromuscular training reduces recurrence 52% at 6 months
- Lopes et al. (Sports Med 2012) · Free PDF: Achilles tendinopathy affects 9–11% of runners (incidence); eccentric loading (Alfredson protocol 2x daily for 12 weeks) achieves 90% clinical success
- Stiell et al. (JAMA 1994, PMID 8271467): Ottawa Ankle Rules: sensitivity 100% for fracture, reduces X-ray use 36% (n=1,032 prospective)
- DiGiovanni et al. (J Bone Joint Surg Am 2003, PMID 12571308): Plantar fascia-specific stretching: 65% excellent results at 8 weeks vs 53% Achilles stretching (n=101 RCT)
- Hupperets et al. (BMJ 2009 · Free PDF, PMID 19542566): Proprioceptive training reduces recurrent ankle sprains 35% over 12 months post-initial sprain (n=522 RCT)
Why Choose Recovery TLV for Ankle Pain
- Licensed physiotherapists trained in Ottawa Ankle Rule assessment
- Functional rehabilitation using evidence-based POLICE model
- Proprioceptive training progression (BAPS board, wobble board, unstable surfaces)
- Eccentric loading protocols for Achilles and plantarflexor strengthening
- Sport-specific return-to-activity programming
- Chronic ankle instability prevention through neuromuscular training
Frequently Asked Questions
Do I need an X-ray for my ankle sprain?
How long does a sprained ankle take to heal?
What causes chronic ankle instability?
Is Achilles pain the same as plantar fasciitis?
Can I run with ankle pain?
Proprioception Retraining and Chronic Ankle Instability Prevention
The single most important factor preventing recurrent ankle sprains is proprioceptive retraining — restoring the mechanoreceptor function of the lateral ligaments and peroneal muscles that was disrupted by the initial sprain. Mechanoreceptors in the ATFL provide real-time sensory feedback to the peroneus longus and brevis, enabling pre-activated muscle stiffness during sudden inversion. After a Grade II-III sprain, this afferent feedback is disrupted for 6-8 weeks even after pain resolves, creating a "proprioceptive gap" during which re-sprain risk is highest.
Proprioceptive training progression: (1) single-leg balance on firm surface — eyes open, then eyes closed; (2) single-leg balance on foam/wobble board; (3) hopping and landing tasks on single leg; (4) sport-specific cutting and direction-change drills. Hupperets et al. (BMJ 2009 · Free PDF, n=522 RCT) demonstrated that a 8-week proprioceptive training program following ankle sprain reduces recurrent sprain rate by 35% over 12 months compared to no intervention. At Recovery TLV, this protocol is integrated into Phase 3 of ankle rehabilitation for all moderate-to-severe sprains, regardless of patient age or activity level.
Related conditions we treat
Get Back to Full Activity Without Fear
Don't let ankle pain limit your athletic performance or daily life. Our functional rehabilitation protocol ensures rapid, safe return to sport. 40% of people develop chronic instability without proper treatment — let us prevent that. Book now.
Clinical information · Recovery TLV
WHAT IS IT — Ankle pain encompasses lateral ligament complex injuries (ATFL, CFL, PTFL — 85% of ankle sprains), Achilles tendinopathy (midportion vs insertional), plantar fasciitis (10% lifetime prevalence), and chronic ankle instability (CAI — 40% of inadequately rehabilitated sprains, Gribble et al. 2016). Ottawa Ankle Rules: sensitivity 100%, specificity 40%, reduces X-rays 36% (Stiell et al., JAMA 1994). Grade III sprain: positive Anterior Drawer Test (sens 85% at day 4-5) and Talar Tilt.
WHO IT AFFECTS — Ankle sprains: 1 per 10,000 per day (most common sports injury). CAI: 40% of lateral sprains. Plantar fasciitis: 10% lifetime, 1-2 million US visits/year. Achilles tendinopathy: 6-18% of runners. In Tel Aviv: runners, padel/tennis players, basketball players, and dancers are common presentations.
HOW WE TREAT IT — Recovery TLV follows POLICE protocol (Protection, Optimal Loading, ICE, Compression, Elevation) — functional treatment returns patients 7 days faster than immobilisation (Kerkhoffs et al., Cochrane 2012). Phase 1: POLICE, pain-free ROM. Phase 2: closed-chain strengthening, proprioception. Phase 3: SEBT progression, sport-specific. Phase 4: return-to-sport (pain <2/10 hopping, 20+ single-leg calf raises). Chronic instability: peroneal EMG biofeedback, neuromuscular training reduces recurrence 52%.
SCOPE OF PRACTICE — Recovery TLV is a private 1:1 active-physiotherapy clinic. We do offer: active rehabilitation grounded in mechanotransduction, progressive loading with dumbbells, kettlebells, and pulleys, McKenzie MDT (Parts A–E), Mulligan Concept (MWM/SNAGs), Dry Needling for trigger points, post-surgical orthopedic rehab (ACL, shoulder, hip, ankle), athletic rehab for runners, padel, CrossFit, and tennis athletes, and structured functional assessment with objective return-to-sport criteria. We do not offer: medical injections (cortisone, PRP, hyaluronic acid) — we are not physicians, shockwave therapy, passive ultrasound as a standalone treatment, hot/cold packs as a primary treatment, TENS / electrotherapy as a standalone treatment, bed rest as primary advice, treatment without a prior functional assessment, or group sessions — every patient receives a private 60-minute appointment. Address: Yaakov Apter 9, Tel Aviv · MoH license 10-120163.
Scientific references
Scientific References (20 peer-reviewed sources)
Curated systematic reviews and meta-analyses from PubMed. All citations include DOI and PubMed ID for verification.
- Shahsanaei Z et al.. Aquatic vs. hopping exercises: A novel comparison of their impacts on motor and sensorimotor rehabilitation in chronic ankle instability. J Bodyw Mov Ther. 2025. PMID:41927248 ·
- Mohamadi S et al.. Neuromuscular control in chronic ankle instability, copers and healthy subjects during dynamic discrete tasks: A systematic review and meta-analysis. J Bodyw Mov Ther. 2025. PMID:41927175 ·
- Bahadori A et al.. Comparison of the effects of combined ankle and lumbopelvic manipulation versus ankle manipulation on static and dynamic balance in patients with chronic ankle instability. J Bodyw Mov Ther. 2025. PMID:41927166 ·
- Jaffri A. Mental Health Predictors of Dynamic Balance in Individuals With Chronic Ankle Instability. J Foot Ankle Res. 2026. PMID:41913085 ·
- Chen P et al.. Effects of hip strengthening on postural control and muscle strength in individuals with chronic ankle instability: A systematic review and meta-analysis of randomized controlled trials. Complement Ther Med. 2026. PMID:41825489 ·
- Zarei S et al.. Aquatic Exercise Enhances Functional Movement and Sensorimotor Performance in Athletes With Chronic Ankle Instability: A Randomized Controlled Trial. J Sport Rehabil. 2025. PMID:40983315
- Wang J et al.. Anatomy changes, signalling pathways, and clinical treatment after ankle sprain. Bone Joint Res. 2026. PMID:42028630 · Free PDF · DOI
- Oh M et al.. Stroboscopic Glasses in Rehabilitation Improve Force Accuracy and Reduce Visual Reliance in Chronic Ankle Instability. J Sport Rehabil. 2025. PMID:40789573 ·
- Steinberg N et al.. Disorganised Achilles tendon structure, chronic ankle instability and reduced neuromuscular abilities in infantry training. BMJ Mil Health. 2026. PMID:42009482 ·
- Daigre J. Peroneal Longus to Brevis Transfer Augmentation With TeKBrace Synthetic Graft. Foot Ankle Spec. 2026. PMID:42007849 ·
- Xu JS et al.. Exercise Therapy for Chronic Ankle Instability: Which Modality for Which Deficit? A Systematic Review and Meta-Analysis. J Foot Ankle Res. 2026. PMID:41771785 · Free PDF ··
- Hu L et al.. Neuromuscular electrical stimulation improves stability and function in chronic ankle instability: a systematic review and meta-analysis. BMC Musculoskelet Disord. 2026. PMID:41992187 ·
- Wu K et al.. Determinants of surgical necessity in Danis-Weber a lateral malleolus fractures: Prognostic insights from a nonoperative cohort. Injury. 2026. PMID:41962195 ·
- Parameyong A et al.. Assessing Balance in Young Athletes With and Without Chronic Ankle Instability. Int J Sports Phys Ther. 2026. PMID:41939964 · Free PDF ·
- Katsuya M et al.. Short-Foot Exercises Improve Postural Control and Ankle Instability in Chronic Ankle Instability: A Randomized Controlled Trial. J Athl Train. 2026. PMID:41938328 · Free PDF ·
- Nguyen AP et al.. Reproducibility of a modified posterior talar glide test in ankle sprain conditions: a cross-sectional analysis on chronic ankle instability, copers, and healthy controls. J Man Manip Ther. 2025. PMID:40635166 ·
- Seyhan S et al.. Injury prevention relevance: markerless functional performance testing in athletes with chronic ankle instability to inform recurrent sprain risk screening. BMC Sports Sci Med Rehabil. 2026. PMID:41906131 · Free PDF ·
- Tsartsapakis I et al.. Manual Therapy, Core Training, and Pilates Method Interventions in Dance Rehabilitation: A Scoping Review. Healthcare (Basel). 2026. PMID:41975874 · Free PDF
- Oh M et al.. Differences in neuromechanics during walking in individuals with bilateral and unilateral chronic ankle instability. J Electromyogr Kinesiol. 2026. PMID:41931946 ·
- Chen P et al.. Effects of Physical Therapy on Proprioception in Individuals with Chronic Ankle Instability: A systematic review with pairwise and network meta-analyses. Am J Phys Med Rehabil. 2026. PMID:41955546 ·