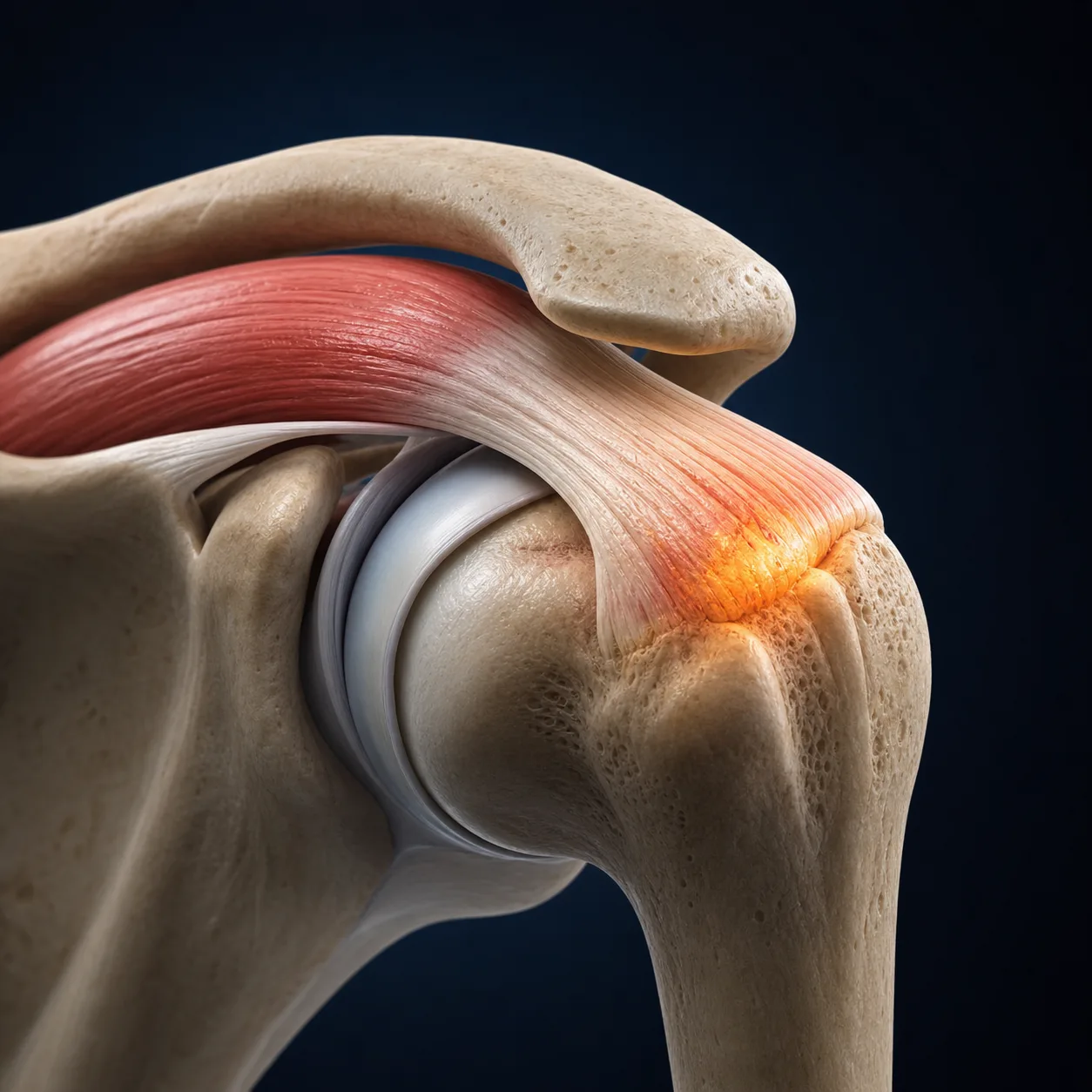
The Rotator Cuff — Four Muscles, One Shoulder
The rotator cuff consists of four key muscles—supraspinatus, infraspinatus, teres minor, and subscapularis—that coordinate to stabilize the shoulder joint. Imbalances, weakness, or overuse in these muscles lead to poor movement mechanics, friction under the acromion, and subsequent rotator cuff tears or tendinopathy that require targeted exercise therapy.
The rotator cuff is a group of four muscles that wrap around the humeral head, providing dynamic stability and powering shoulder rotation. Understanding which muscle is affected — and why — is the foundation of targeted rehabilitation.
Supraspinatus
Initiates arm elevation (first 30°). Most commonly involved in both impingement and tears. Tested with the Jobe empty-can test.
Infraspinatus
Primary external rotator. Weakness leads to superior humeral migration and SAPS. Key muscle in throwing athletes. Tested with ER lag sign.
Teres Minor
Assists infraspinatus in ER and depresses the humeral head. Often overlooked; critical in overhead sports rehabilitation and instability cases.
Subscapularis
Largest RC muscle. Primary internal rotator and anterior stabiliser. Tears occur with forced ER or anterior dislocation. Tested with belly-press and lift-off tests.
A useful mnemonic is SITS (Supraspinatus, Infraspinatus, Teres minor, Subscapularis). Together, they compress the humeral head against the glenoid — a mechanism called the concavity-compression effect. When any of these muscles is weak or inhibited, the joint loses centration, increasing load on the bursa and labrum.
Common Shoulder Conditions We Treat
Physiotherapy effectively treats a wide range of shoulder conditions, including frozen shoulder (capsular stiffness), rotator cuff tears and tendinopathy (lateral arm pain), shoulder impingement, labrum tears (catching and instability), calcific tendinitis, and post-surgical rehabilitation following rotator cuff repairs or labral stabilization procedures.
Subacromial Pain Syndrome (SAPS)
Previously called "shoulder impingement." Irritation of the subacromial bursa and rotator cuff tendons. The most common shoulder complaint. Responds very well to targeted exercise.
Rotator Cuff Tear
Partial or full-thickness tearing of RC tendons — most often supraspinatus. Conservative rehab is first-line; many full-thickness tears improve without surgery, especially in those over 60.
SLAP Lesion
Superior Labrum Anterior to Posterior tear — where the biceps tendon anchors to the socket rim. Common in throwing athletes and after traumatic dislocation.
Frozen Shoulder
Adhesive capsulitis — inflammation and fibrosis of the joint capsule causing severe stiffness. Three stages: freezing, frozen, thawing. Joint mobilisation is highly effective.
Shoulder Instability
Excessive laxity allowing the humeral head to translate excessively — from traumatic dislocation or atraumatic multi-directional instability. Scapular and RC strengthening is the cornerstone.
Post-Surgical Rehab
Structured rehabilitation after RC repair, labral surgery, Bankart repair, or shoulder replacement. Phase-based protocols aligned with tissue healing timelines.
What the Research Says
Clinical trials demonstrate that structured physiotherapy is highly effective for shoulder pain. For rotator cuff tears and impingement, progressive exercise therapy yields long-term outcomes in pain relief and function equivalent to arthroscopic surgery, with significantly lower risk. Early conservative loading is the recommended primary intervention for most shoulder pathologies.
A landmark UK trial (Lewis, BJSM 2014 — the CODA trial) found that structured exercise therapy was equally effective as subacromial corticosteroid injection at 6 months for subacromial pain syndrome. Exercise produced more durable results at 12-month follow-up.
Holmgren et al. (JOSPT 2012) demonstrated that specific RC and scapular strengthening reduced the surgery rate from 63% to just 20% in patients scheduled for acromioplasty — a 3× reduction. The majority avoided the operating table entirely with targeted physiotherapy.
Key clinical insight: "Impingement" has been largely retired as a diagnosis. The current model (Lewis, Br J Sports Med 2016) recognises that pain comes from load-capacity mismatch in the rotator cuff and bursa — not from mechanical pinching. This means loading and strengthening the tendon is the treatment, not avoiding movement.
GIRD — The Hidden Problem in Overhead Athletes
Glenohumeral Internal Rotation Deficit (GIRD) is posterior capsule tightness causing a side-to-side difference in internal rotation greater than 18–20°. It is common in baseball, tennis, volleyball and swimming — any sport with repetitive overhead loading.
GIRD forces the humeral head to posterosuperiorly migrate during the cocking phase of throwing, dramatically increasing stress on the superior labrum and rotator cuff. Treatment: sleeper stretch and posterior capsule joint mobilisation, combined with posterior shoulder strengthening.
Wilk et al. (AJSM 2011): restoring IR range of motion in throwing athletes reduced SLAP and RC injury rates by approximately 38%.
Scapular Dyskinesia
The scapula is the platform from which the rotator cuff operates. Scapular dyskinesia — altered scapular motion and position — is present in the majority of patients with shoulder pain. When the scapula cannot upwardly rotate and posteriorly tilt during arm elevation, the subacromial space narrows and the rotator cuff is overloaded.
Key muscles to retrain: serratus anterior (scapular protraction and upward rotation), lower trapezius (posterior tilt and depression), middle trapezius (retraction). Exercises: wall slides, push-up plus, prone Y-T-W, band pull-apart.
Clinical Tests Used in Assessment
At the initial session we run a structured set of orthopaedic tests alongside movement analysis and strength testing to differentiate between shoulder pathologies:
| Test | Target Structure | Sensitivity / Notes |
|---|---|---|
| Hawkins-Kennedy | Subacromial space / SAPS | High sensitivity (~79%). Internal rotation in 90° flexion. |
| Neer Sign | Supraspinatus / bursa | Forward flexion with arm in internal rotation. Useful with Hawkins. |
| Jobe Empty-Can | Supraspinatus strength/integrity | 90° abduction, 30° horizontal flexion, thumb pointing down. Weakness = RC pathology. |
| ER Lag Sign | Infraspinatus / teres minor tear | High specificity for full-thickness IR/ER tear when positive. |
| O'Brien's Test | SLAP lesion / AC joint | Positive in pronation, negative in supination = SLAP. Both positive = AC joint. |
| Speed's Test | Biceps tendon / bicipital tendinopathy | Resisted forward flexion with elbow extended, palm up. |
| Apprehension-Relocation | Anterior instability | Apprehension in ER with posterior pressure relieving = positive. High specificity. |
5-Phase Shoulder Rehabilitation Programme
Shoulder rehabilitation progresses through five structured phases: Phase 1 controls pain and inflammation; Phase 2 restores passive range of motion; Phase 3 initiates active strengthening of the rotator cuff and scapular stabilizers; Phase 4 develops functional strength and dynamic control; and Phase 5 prepares for full return to sports or manual work.
Rehabilitation is phase-based, with criteria that must be met before advancing to the next stage. Timelines vary by diagnosis and tissue healing rates:
Pain Control & Protection
Reduce acute inflammation. Relative rest from provocative loading. RICE/ice, pain education, gentle pendulum exercises, cervical and thoracic mobilisation to improve neural input. Posture correction begins.
Restore Range of Motion
Passive then active-assisted shoulder flexion, abduction, ER/IR. Capsular stretching (posterior and inferior capsule as indicated). Scapular mobility drills. Thoracic spine extension mobilisation. Begin low-load isometric RC exercises.
Rotator Cuff Strengthening
Isotonic RC loading: side-lying ER (infraspinatus), ER/IR with resistance band (subscapularis), empty-can progression (supraspinatus). Begin scapular stabiliser loading: serratus anterior wall push-up plus, prone T and Y for lower/middle trapezius.
Functional Loading & Scapular Control
Overhead pressing with controlled tempo, cable rows, push-up progressions, prone Y-T-W with load. Dynamic neuromuscular control exercises. Sport-specific loading begins at sub-maximal intensity. ER:IR strength ratio target ≥ 0.66.
Return to Sport / Full Activity
Sport-specific movement patterns at full load. Throwing progression (for overhead athletes): 20–45–60–90 m stepped protocol. Plyometric upper-limb training. Passed criteria: full ROM, symmetrical strength (>90% limb symmetry index), pain-free overhead activity.
Red Flags — seek urgent medical attention if you have: arm or hand numbness/tingling (may indicate C5/C6 nerve root compression), severe night pain without provocation, systemic symptoms (fever, weight loss), acute inability to raise the arm after trauma, or left shoulder and chest pain together (may be cardiac).
Not Sure What's Wrong With Your Shoulder?
A 50–60-minute assessment will give you a clear diagnosis, a clinical explanation of what's causing your pain, and a structured rehabilitation plan.
Frequently Asked Questions
Do I need surgery for a rotator cuff tear?
How long does shoulder rehabilitation take?
What is SLAP and do I need surgery?
What is frozen shoulder and how is it treated?
What is the difference between shoulder impingement and a rotator cuff tear?
Related conditions we treat
Ready to Rehabilitate Your Shoulder?
Private 1:1 sessions · Tel Aviv · Evidence-based protocols · Same-week availability